FATTY LIVER DISEASE (FLD)
Fatty liver disease is a most common liver disease
affecting a wide range of population worldwide. It is caused due to excessive
fat accumulation in liver cells resulting in inflammation in liver. It may share characteristics
with the conditions of Medoroga (obesity) and Yakrit Roga (liver
disorders), where improper diet and lifestyle lead to an imbalance in the
Doshas. This imbalance results in impaired digestion and the accumulation of
Ama, contributing to fat deposition in the liver
Fatty liver mainly develops due to wrong food habits, overeating, junk and oily foods, soft drinks, and a sedentary lifestyle. These causes disturb Agni (digestive fire), leading to the formation of Apakva Anna Rasa (poorly digested food essence).
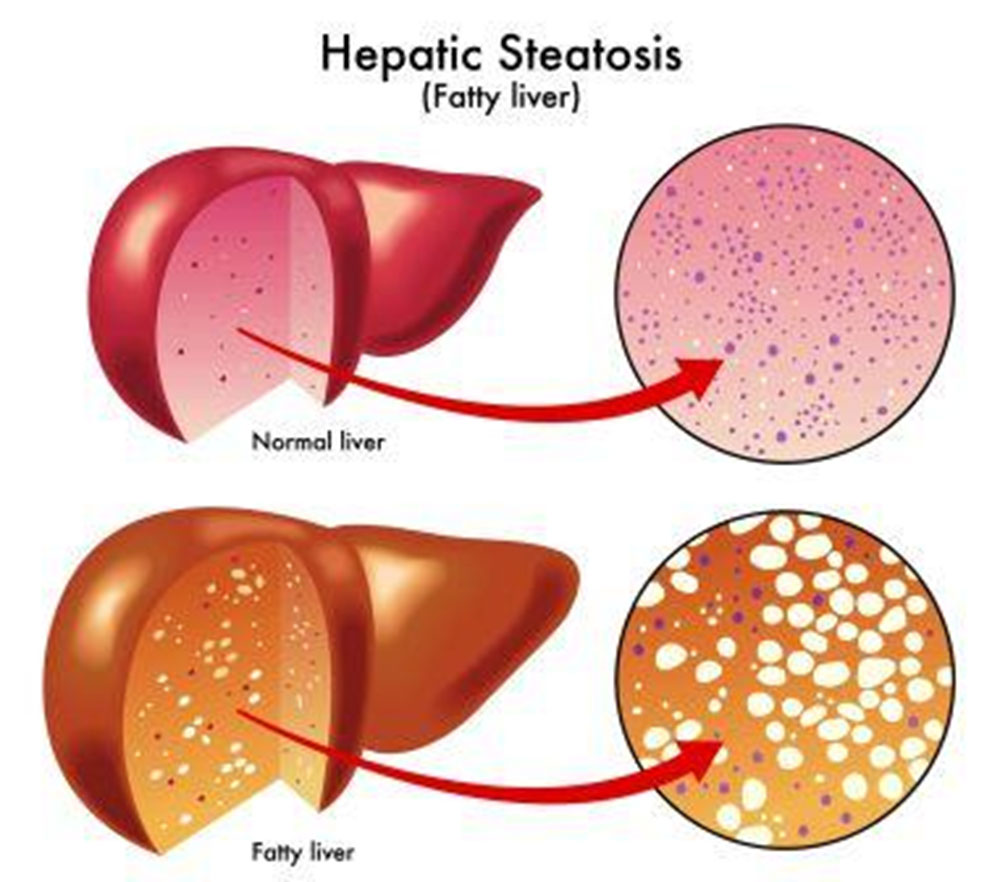
There are two main types:
·
Nonalcoholic fatty
liver disease (NAFLD)
·
Alcoholic fatty
liver disease, also called alcoholic steatohepatitis
Nonalcoholic fatty
liver disease (NAFLD)
NAFLD is a type of fatty liver disease that is not related
to heavy alcohol use. There are two kinds:
1.
Simple fatty
liver: fat in the liver with little or no inflammation or liver cell damage. It
usually does not cause serious complications.
2. Nonalcoholic steatohepatitis (NASH): fat in the liver along with
inflammation and liver cell damage, which can lead to fibrosis, cirrhosis, or
liver cancer
Alcoholic fatty
liver disease
Alcoholic fatty liver disease is caused by heavy alcohol
use. The liver breaks down alcohol, producing harmful substances that damage
cells, promote inflammation, and weaken natural defenses. This is the earliest
stage of alcohol-related liver disease, followed by alcoholic hepatitis and
cirrhosis.
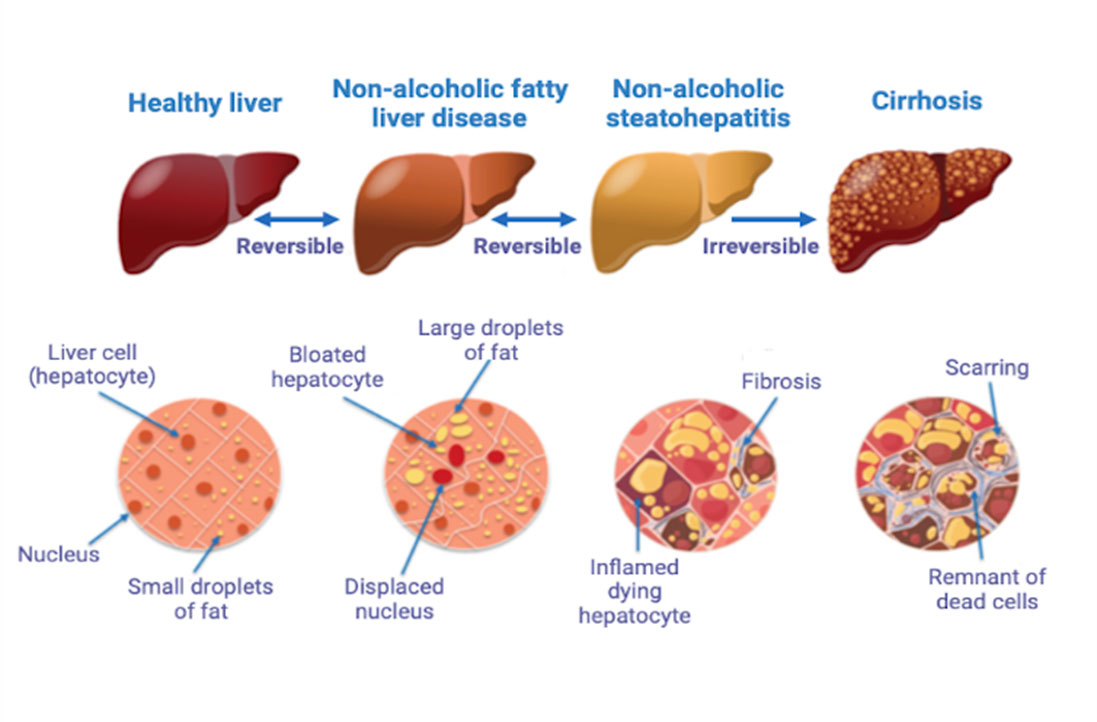
Stages of non-alcoholic fatty liver disease
1: Fatty liver
(steatosis) -The 1st stage, where
there is build-up of fat but no damage to your liver
2: Non-alcoholic
steatohepatitis (NASH) -A
build-up of fat has caused inflammation in your liver. It is not yet seriously
damaged, but there's a risk it could get worse
3: Fibrosis -There is damage to your liver, but it will
usually still be working well. It's important to try to stop further damage
which could lead to cirrhosis
4 Cirrhosis -There is severe damage to your liver that will affect how well it works. This could cause serious health problems including internal bleeding, liver failure, liver cancer or sepsis
Ayurvedic view
Non-Alcoholic Fatty Liver Disease (NAFLD) can
be correlated in Ayurveda with Yakritodara and Pleehodara, which are described
under Udara Roga. It is considered a Santarpanajanya Vyadhi, caused by
over-nutrition and lack of physical activity. Due to Kapha and Meda dushti,
along with Agnimandhya, improper digestion occurs leading to Ama formation and
Srotorodha. This results in fat accumulation in the liver. As the disease
progresses, Pitta dushti causes inflammation similar to NASH, and long-standing
Vata prakopa leads to fibrosis and cirrhosis
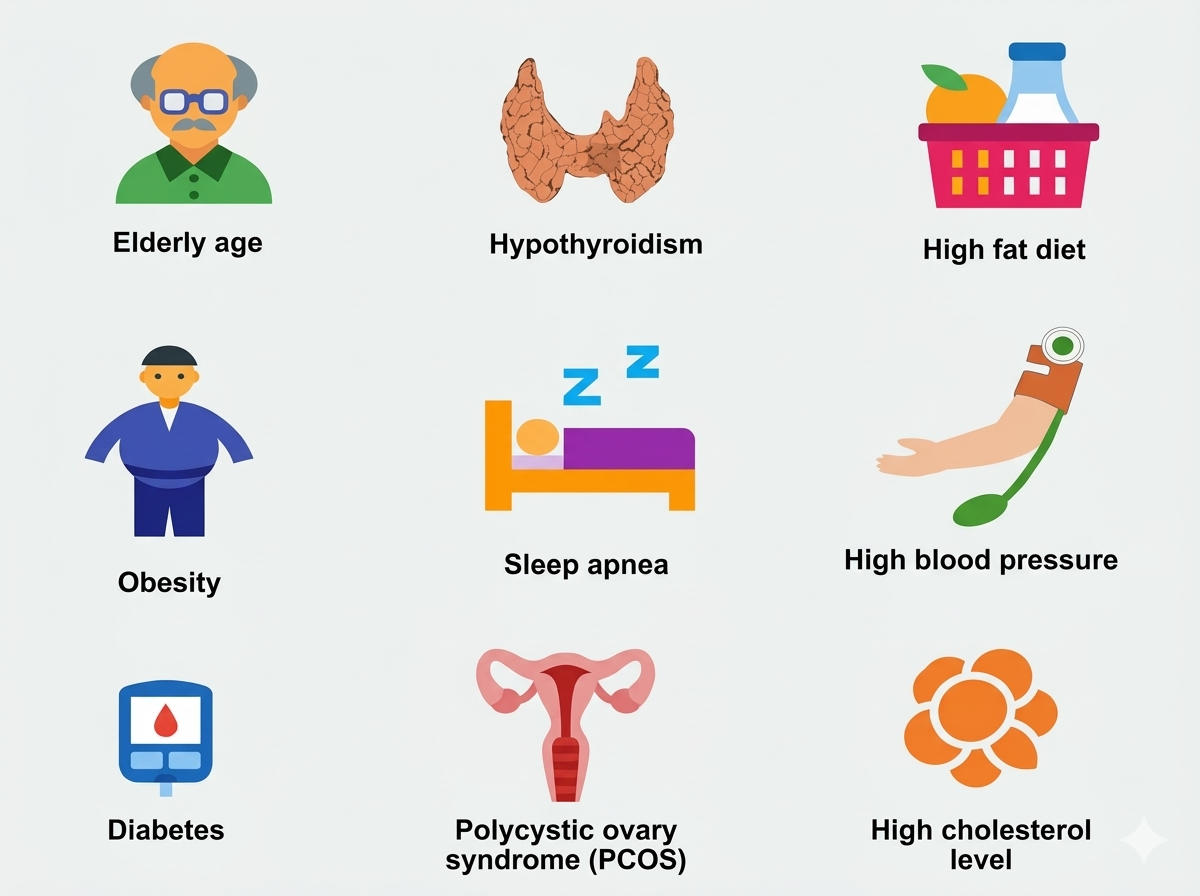
Risk Factors of Fatty Liver Disease (NAFLD)
-Obesity
-Type
2 diabetes mellitus
-Insulin
resistance / Prediabetes
-Metabolic
syndrome
-High
triglycerides
-High
blood pressure (Hypertension)
-Sedentary
lifestyle / physical inactivity
-Middle
age and older age
-Rapid
weight loss or malnutrition
-Certain
medications (e.g., corticosteroids)
-Polycystic
ovary syndrome (PCOS)
-Hypothyroidism
-Genetic predisposition / family history
Symptoms of Fatty Liver Disease
Early / Common Symptoms
-Fatigue
and weakness – feeling tired or low in energy
-Malaise
– general feeling of being unwell
-Right
upper abdominal discomfort – dull ache or heaviness
-Loss
of appetite
-Mild,
unexplained weight loss
Many
patients are asymptomatic in early stages.
Symptoms of Advanced Disease (NASH /
Cirrhosis)
-Jaundice
– yellowing of skin and eyes
-Ascites
– fluid accumulation in the abdomen
-Peripheral
edema – swelling of legs and feet
-Pruritus
(itchy skin)
-Dark-colored
urine and pale stools
-Easy
bruising or bleeding
-Spider
angiomas (spider veins)
-Palmar
erythema – redness of palms
-Hepatic encephalopathy – confusion, memory loss, personality changes

Diagnosis
-Medical
history (including alcohol use, medications)
-Physical
examination (weight, enlarged liver, jaundice)
-Blood
tests (liver function, blood count)
-Imaging
tests (fat in liver, stiffness = fibrosis)
-Liver
biopsy (to confirm severity)
Management of
fatty liver disease
Ayurvedic Management of NAFLD offers a comprehensive
strategy by focusing on improving liver functions, reducing oxidative stress,
and boosting metabolism. Fatty liver disease is initially managed with dietary
restriction, regular physical exercise, and weight reduction. In Ayurveda,
management focuses
1.
Correcting digestion
(Agnivikṛti) :
Fixing your “digestive fire “ so food turns into energy instead of fat
2.
Reducing vitiated
Kapha and Meda: clearing out excess mucus like energy and body fat
3.
Opening channels (Srotorodha):
Removing blockages in the body’s pathways to let fluids and energy flow freely by
pacifying Vata through Agnidipana and Rukṣaṇa,
4.
Deep cleaning
(shodhana): Sometimes the body needs a “reset” through detoxification.
Virechana is the preferred sodhana therapy in liver disorders as it eliminates
excess Pitta Doṣa,
improves appetite, and enhances liver function, while Vamana is useful in obese
patients for reducing body weight and lipid levels.
5.
Samana Chikitsa
includes hepatoprotective herbs such as Bhumyamalai ( A powerful liver tonic),
Kaṭuki (Known for
clearing gallbladder and liver
congestion) , Guḍuci(
Boosts immunity and reduces inflammation)
, and Haritaki ( Helps with gentle daily cleansing) , along with classical
formulations like Decoctions (Kashaya),Tonics ( Ariṣṭa), Powders (Churṇa), and Ghee(Ghṛta).
6.
Ahara (Food)
should be light, easily digestible, low in fat and carbohydrates, Kapha-Meda
reducing, and include warm, freshly prepared food while avoiding oily, fried,
sugary, and heavy meals, alcohol, and junk food.
7.
Vihara (Habits ) includes regular physical
activity, daily walking, yoga, avoidance of day sleep, maintenance of proper
sleep–wake routine, stress reduction, and adoption of a disciplined lifestyle
to support digestion and liver function.
Ayurvedic management of alcoholic fatty liver focuses on
detoxifying the liver, correcting metabolism (Agni), and reducing inflammation
through Panchakarma specifically nitya virechana (daily therapeutic purgation) often preceded by Snehapana (internal
oleation) and Swedana (sudation), hepatoprotective herbs (e.g., Bhumiamalaki,
Guduchi, Kutaki), and lifestyle modifications.
Dr Murshida Chemmukkan (B.A.M.S)
Medical Officer
Dr. P. Alikutty's Ayurveda and Modern Hospital – Kottakkal
 en
en
 العربية
العربية